Boom-Bust: The Cycle Keeping Your Injury Going
What is the Boom/Bust Cycle?
We've all been there - that persistent niggling in the achilles or pain in the shoulder finally feels normal! Excited to get back in the swing of things, we jump back in - swim a full workout, or go for a run on our favorite route. The next day, it's like we're back at square one. We flounder through the whole process again, from the mess of exercises and massage we're not sure are actually helping, all the way back to that fateful day when it feels better. Then, like clockwork, we fall for it again.
As a physical therapist for endurance athletes like swimmers, runners, and cyclists I see this kind of cycle all too commonly. In fact, it's so common that it has a name: the boom-bust cycle [Psychology Tools; NSW Agency for Clinical Innovation]. But why is it so common? Several psychological and physiological factors make this type of pattern particularly difficult to break - from the way our tissues really heal, to the way that our memories work.
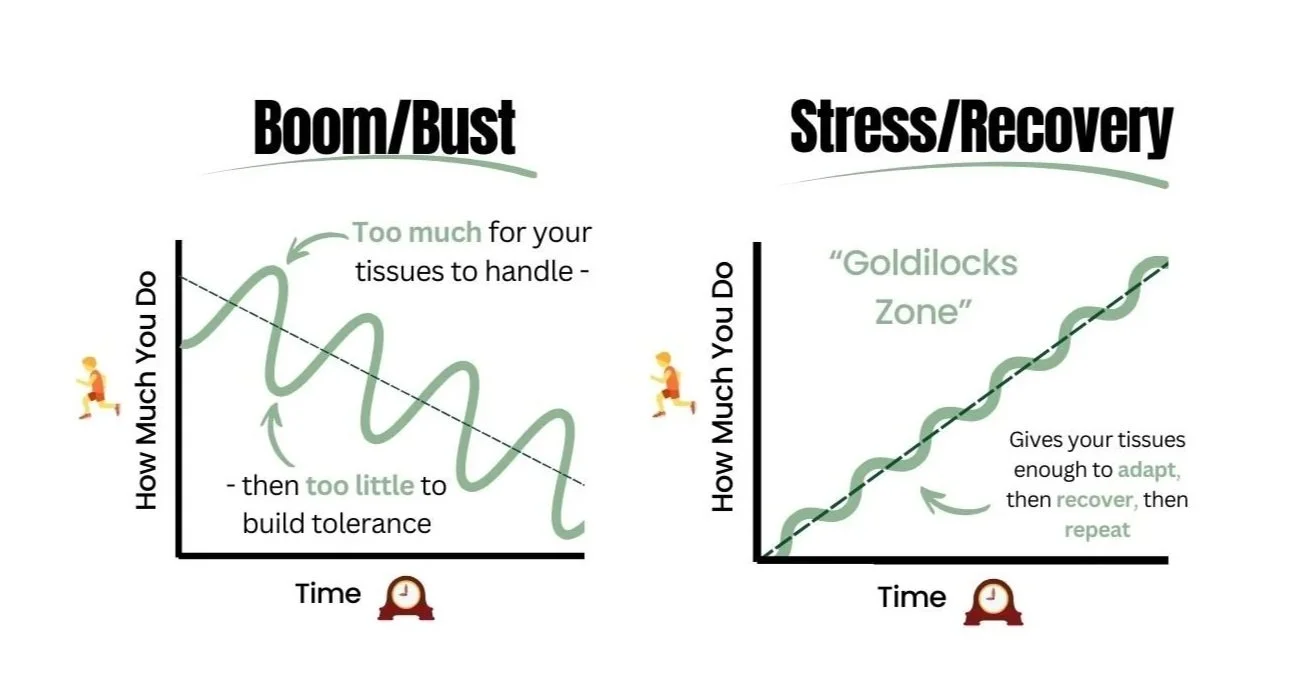
A visual representation of the cycle - and its opposite, the stress-recovery cycle.
Absence of Pain ≠ Healing
One key aspect to the boom-bust cycle is the erroneous belief that we can ONLY exercise when we're not in pain - and that once the pain is gone, that means the tissue has healed and we're "good to go" at our normal levels. In truth, pain and healing do not correlate neatly [Physiopedia – Tendinopathy Rehabilitation]. In fact, having some pain during the recovery process for many issues such as tendinopathies is normal, even essential - it means you're stressing the area enough to make healing adaptations occur [Apunts Sports Medicine – Load Management in Tendinopathy]. Being ok with low level pain during recovery means that we can gradually increase the volume of exercise we're engaging in - think running only a couple extra minutes each session. When we do that, we stay within the "envelope of function" - the lowest level that we continue to work at without surpassing our threshold (the "bust" part) [Wiegerinck et al. – Conservative Management of Achilles Tendinopathy; OSU Wexner Medical Center CPG].
Another aspect of the boom-bust cycle that keeps it going is our situational memory. If we believe that lack of pain = safety, we'll selectively remember our past experiences supporting that idea - and continually find out that it's incorrect [Psychology Tools]. Sticking with the process of gradual increase becomes essential - trusting in the process rather than what we wish to believe [E3 Rehab – Patellar Tendinopathy Guide].
Over-reliance on Exercise
That wishing to believe we're totally better brings us to a final point that perpetuates the boom-bust cycle: so many endurance athletes rely in an outsize way on their exercise for stress management. If they "don't get in a workout, they have a bad day." When a vigorous workout is the only way you can feel at ease, you'll likely find ways to rationalize to yourself why it's ok to do: "this time, I'm totally healed! It'll be fine!" Learning different ways to regulate emotion and stress become a crucial part of the rehab process [PMC – Exercise Addiction in Endurance Athletes; PMC – Effects of Stress on Physical Activity].
Take Charge
The boom-bust cycle is common, and once understood seems like the most obvious thing in the world. Overcoming it, however, can be incredibly difficult. It requires intense honesty with oneself, and looking in a mirror in a way that can feel uncomfortable. That's where a professional like a Doctor of Physical Therapy comes in. We don't just provide knowledge - LLMs and PubMed can do that. We're accountability partners, coaches, and movement experts all in one. If you recognize yourself in this type of cycle, I help runners, swimmers, and cyclists overcome these same challenges all the time. Schedule an appointment, I'd love to talk.
🌐 Homepage
References
Psychology Tools. Pacing for Pain and Fatigue. https://www.psychologytools.com/resource/pacing-for-pain-and-fatigue
NSW Agency for Clinical Innovation. Boom and Bust Cycle. https://aci.health.nsw.gov.au/chronic-pain/brain-injury/fatigue/boom-and-bust
Physiopedia. Tendinopathy Rehabilitation. https://www.physio-pedia.com/Tendinopathy_Rehabilitation
Apunts Sports Medicine. Load Management in Tendinopathy. https://www.apunts.org/en-load-management-in-tendinopathy-clinical-articulo-S1886658117300580
Wiegerinck et al. Conservative Management of Achilles Tendinopathy. PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC7249277/
OSU Wexner Medical Center. Tendinopathy Clinical Practice Guideline. https://wexnermedical.osu.edu/-/media/files/wexnermedical/patient-care/healthcare-services/sports-medicine/education/medical-professionals/other/tendinopathy.pdf
E3 Rehab. Patellar Tendinopathy Guide. https://e3rehab.com/patellartendinopathy/
PMC. Exercise Addiction in Endurance Athletes. https://pmc.ncbi.nlm.nih.gov/articles/PMC12306302/
PMC. Effects of Stress on Physical Activity. https://pmc.ncbi.nlm.nih.gov/articles/PMC3894304/